Poor Posture and Lower Back Pain: What’s the Link?
Poor Posture Lower Back Pain: Causes, Symptoms and What May Help
If you have poor posture and lower back pain, you’re not alone. Many Australians notice their lower back feels stiff, sore or “tight” after a day at the desk, driving, or standing for long stretches. While posture isn’t the only factor in back pain, sustained positions and repetitive habits can contribute to discomfort for some people.
The helpful takeaway is this: it’s usually not about finding “perfect posture”. It’s about reducing load on sensitive areas, building tolerance gradually, and adding more movement variety into your day.
What do we mean by “poor posture”?
“Poor posture” usually describes positions that are held for a long time and don’t suit your body’s current capacity. Common examples include:
Slouching or collapsing through the lower back while sitting
Sitting with the pelvis tucked under (tailbone “rolled under”)
Standing with weight mainly on one leg
An exaggerated arch in the lower back (often with ribs flared forward)
Long periods of stillness (even if you look “upright”)
Importantly, a posture isn’t automatically bad. The same position can feel fine for 10 minutes and uncomfortable after 2 hours. Duration and repetition matter.
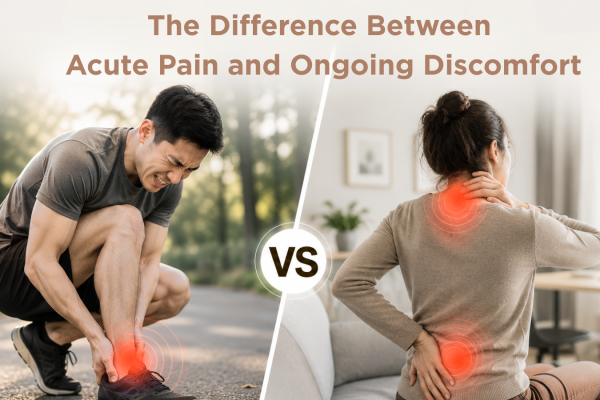
The link between poor posture and lower back pain
Lower back pain is complex and can be influenced by many factors, including stress, sleep, activity levels, previous injuries, strength, and general health. That said, poor posture can be one piece of the puzzle for some people, particularly when it leads to:
1) Increased strain from sustained loading
When you sit or stand in the same position for a long time, certain joints and tissues can become loaded repeatedly. Over time, this may contribute to:
local muscle fatigue
joint stiffness
“tightness” around the hips and lower back
a dull ache that builds as the day goes on
This is why lower back pain from sitting is such a common complaint.
2) Muscle guarding and tension
If your body senses a position is uncomfortable or unstable, it may respond by tightening muscles around the area to protect it. This “guarding” can feel like:
tight lower back muscles
sore glutes
tension through the hips or hamstrings
reduced range of motion when you try to move
Guarding isn’t dangerous on its own, but it can be tiring and uncomfortable.
3) Reduced movement options
Posture becomes more of an issue when it limits movement variety. For example, if your day involves:
commuting
desk work
couch time
then sleep in a curled position
…your lower back may simply be spending too many hours in flexion (rounded positions) with too little variety.
4) Hips and pelvis doing the heavy lifting
The pelvis sits between the hips and the lower back. When posture habits shift pelvic position (for example, a tucked-under slouch or an excessive arch), it can change how the lower back and hips share load.
You might hear terms like:
anterior pelvic tilt (more arch)
posterior pelvic tilt (more tuck)
These aren’t “good” or “bad” by themselves, but they can be relevant if a position consistently aggravates your symptoms.
Signs your posture may be contributing
Posture may be part of your lower back pain picture if you notice:
pain that builds during sitting or standing and eases with movement
stiffness when you first stand up after sitting
a “locked” or tight feeling in the lower back after desk work
symptoms that improve on holidays or weekends when you move more
one-sided ache linked to always leaning to the same side
If your pain is severe, persistent, or worsening, it’s worth getting an individual assessment rather than guessing.
What to do about it (practical, realistic steps)
1) Aim for “next posture”, not “perfect posture”
The best posture is usually the one you don’t stay in for too long. Try changing position every 20 to 40 minutes when possible:
stand up for 30 to 60 seconds
take a short walk to the kitchen
do a gentle back bend or hip stretch (only if comfortable)
reset your sitting position
Small changes, done consistently, often beat big changes done once.
2) Adjust your desk setup to reduce strain
A few basics that help many people:
Feet supported (flat on the floor or on a footrest)
Hips slightly higher than knees (often helps reduce slumping)
Screen at eye level so you’re not rounding forward
Keyboard and mouse close to avoid reaching
Consider a small lumbar support (a rolled towel can work)
If you use a sit-stand desk, aim for variety rather than standing all day.
3) Build tolerance with simple strength work
When the lower back is sore, people often focus only on stretching. Stretching can feel good, but long-term comfort often improves when you also build capacity in key areas:
glutes
legs
trunk (core and back muscles)
upper back strength to support sitting posture
A simple starting point (if comfortable) might include:
sit-to-stands from a chair
bridges
supported squats
gentle bird-dog holds
short daily walks
If you’re unsure what’s appropriate for your situation, a clinician can tailor this based on your symptoms and history.
4) Watch the “big rocks”: sleep, stress, and activity
Back pain is rarely just mechanical. You may notice posture hurts more when you’re:
run down
stressed
sleeping poorly
doing less movement overall
Improving sleep routine, gradually increasing activity, and managing workload can all support recovery.
5) Know when to seek help
Consider booking an assessment if:
pain lasts longer than 2 to 3 weeks without improvement
it keeps returning or limits your work, exercise, or sleep
you’re unsure what movements are safe for you
pain is accompanied by pins and needles, numbness, or leg symptoms
you want a plan that’s specific to your body and lifestyle
A chiropractor or other musculoskeletal professional can assess how your spine, hips, and surrounding muscles are functioning, and help you build a practical plan. Treatment may include hands-on care, mobility work, and exercise advice, depending on your needs.
Red flags: seek urgent medical advice
Seek urgent medical help if you have new or worsening:
changes to bladder or bowel control
significant weakness in the legs
numbness in the groin/saddle area
fever, unexplained weight loss, or pain after major trauma
FAQ
Can poor posture cause lower back pain?
It can contribute for some people, especially when a posture is held for long periods and your body isn’t tolerating the load well. Often it’s the combination of posture, reduced movement, and overall capacity that matters.
Should I sit up straight all day?
Not usually. Holding a rigid “perfect posture” can be tiring. A better goal is to change positions regularly and set up your workspace so sitting is easier on your body.
Is stretching enough to fix posture-related back pain?
Stretching can help temporarily, but many people do better with a combination of movement breaks, strength, and ergonomic changes, based on their individual presentation.
Can a chiropractor help with posture-related lower back pain?
After an appropriate assessment, chiropractic care may help by improving mobility, reducing discomfort, and guiding you with posture and exercise strategies tailored to your situation. Results vary and depend on individual factors.
If you’re dealing with poor posture and lower back pain that keeps coming back, a personalised assessment can help clarify what’s driving your symptoms and what’s likely to help. Wellbeing Chiropractic has clinics across Melbourne, with locations also in Sydney and Brisbane. If you’d like support, you can book an appointment and we’ll work with you on a plan that fits your body, routine and goals.
Author